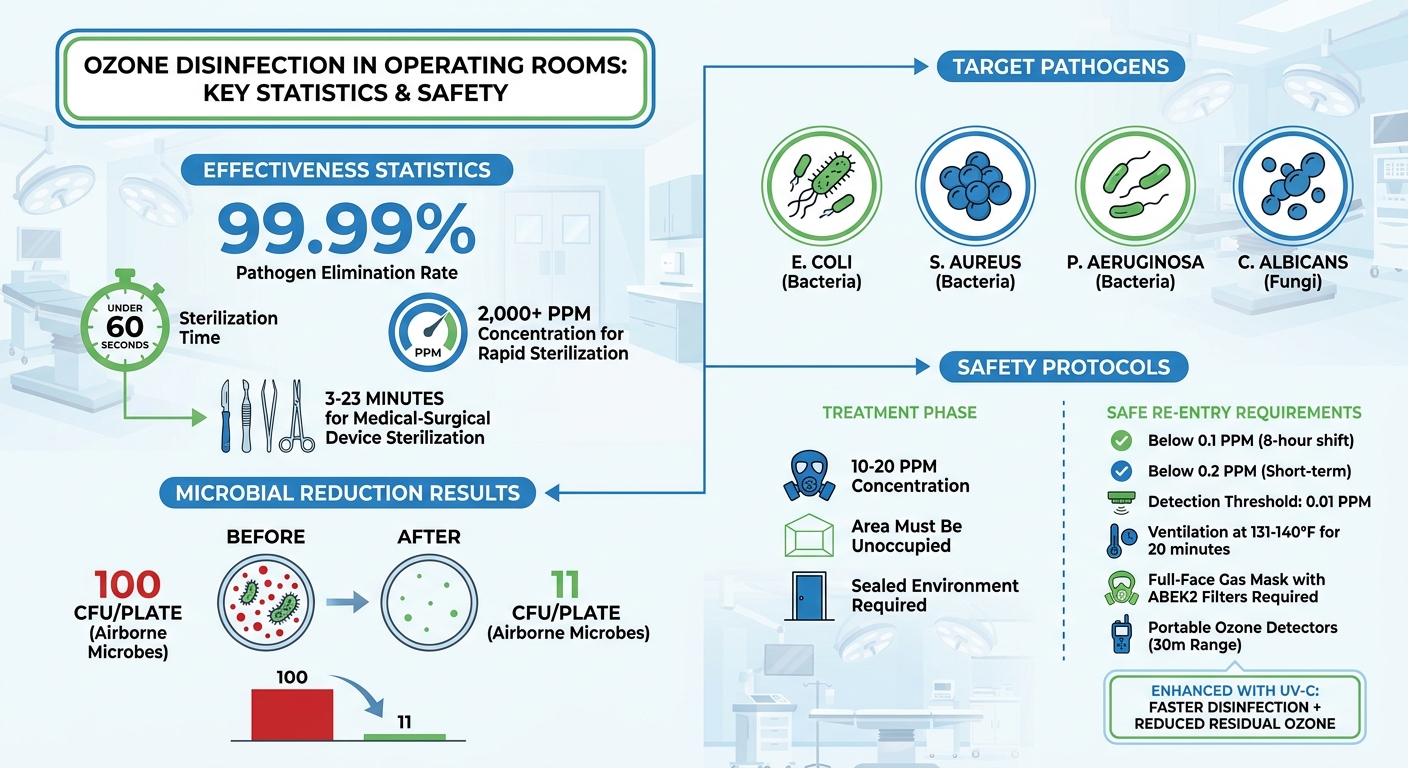
Ozone disinfection is proving to be a highly effective method for sterilizing operating rooms. Recent research shows it eliminates over 99.99% of harmful pathogens, including bacteria like E. coli and fungi such as Candida albicans, in under 60 seconds. By using ozone gas (O₃) as a powerful oxidizing agent, it reaches areas traditional cleaning methods often miss, such as ventilation systems and equipment crevices.
Key insights include:
- High Efficiency: Ozone concentrations above 2,000 ppm sterilize surfaces and air in minutes.
- Safety Protocols: Strict measures, like ventilation and specialized protective gear, are necessary to ensure safe use.
- Enhanced Techniques: Combining ozone with UV-C technology accelerates disinfection and reduces residual ozone.
While ozone disinfection offers a fast and thorough cleaning solution, proper management and safety precautions are critical to protect healthcare staff and equipment. This method is gaining traction as an effective addition to operating room hygiene practices.
Ozone Disinfection Effectiveness and Safety Guidelines for Operating Rooms
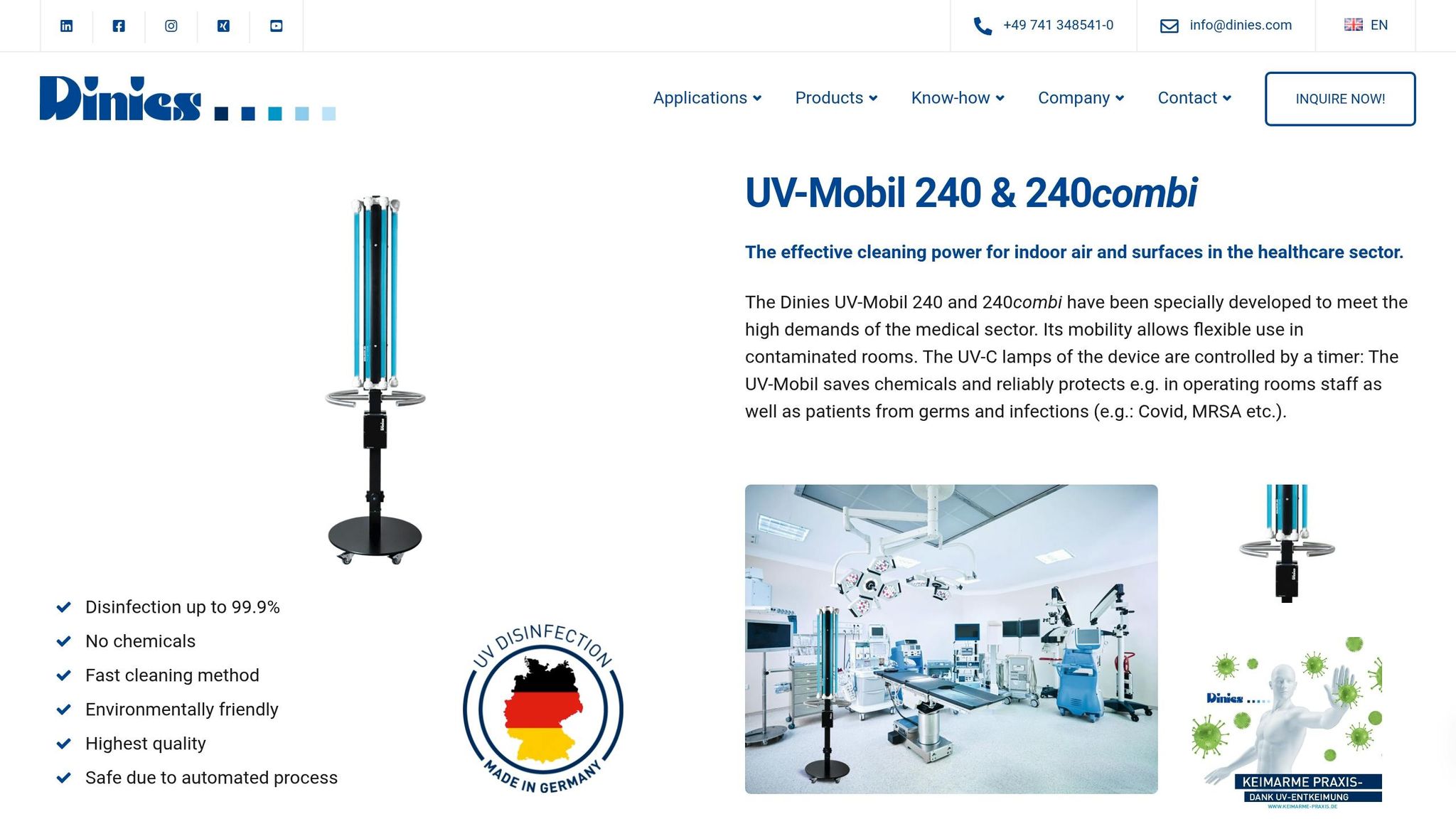
Dinies UV-Mobil 240 combi: The automated 360° disinfection with UV-C light and ozone
sbb-itb-5fea4da
What the Research Shows About Ozone Disinfection
Studies continue to highlight ozone’s ability to reduce both airborne and surface microbes, with its effectiveness depending on the concentration and duration of exposure. Here’s a closer look at some key findings that demonstrate its potential.
Study 1: Airborne and Surface Microbial Reduction
Research has shown that ozone treatment significantly lowers airborne microbial counts. For instance, one study found microbial levels dropped from 100 CFU/plate to just 11 CFU/plate after ozone exposure. This highlights its usefulness in areas where traditional cleaning methods might fall short.
Study 2: High-Intensity Ozone in Medical Settings
In hospital environments, high-intensity ozone applications (exceeding 2,000 ppm) have proven to sterilize medical-surgical devices in as little as 3 minutes and up to 23 minutes. This method has been effective against a wide range of pathogens, including E. coli, S. aureus, P. aeruginosa, and fungi such as C. albicans.
Study 3: Ozone Combined with UV-C Technology
Using ozone alongside UV-C technology has shown promising results in neurorehabilitation rooms. This combination not only enhances disinfection in enclosed spaces but also quickly converts leftover ozone into oxygen, reducing wait times and ensuring a safer environment for healthcare workers. This dual approach emphasizes both efficiency in pathogen removal and safety for operators.
How Ozone Concentration and Exposure Time Affect Results
The success of ozone disinfection depends heavily on two factors: the concentration of ozone and the duration of exposure. In high-risk environments like operating rooms, where the atmosphere is tightly controlled, disinfection must be precise. The process typically involves several stages: cleaning before procedures, sanitizing between procedures, and performing a thorough disinfection at the end of the day.
Getting the balance right between ozone levels and exposure time is key to achieving thorough pathogen elimination in these critical settings. This careful calibration ensures disinfection is both effective and efficient.
Safety Measures for Ozone Disinfection
When using ozone disinfection in operating rooms, adhering to strict safety protocols is essential to protect both personnel and equipment. The process typically involves ozone concentrations of 10–20 ppm, which are dangerous to humans. Therefore, it’s critical that these areas remain unoccupied during treatment. Afterward, thorough ventilation or air recycling must be conducted to eliminate any remaining ozone safely. For more information on the process, see our disinfection service FAQs.
While ozone can be detected by its smell at concentrations as low as 0.01 ppm, relying on odor alone is not enough to ensure safety. Operators must verify that ozone levels are below 0.1 ppm for an 8-hour work shift or 0.2 ppm for short-term exposure. Portable ozone detectors are indispensable for this task, with some models offering remote monitoring capabilities for distances up to 30 meters.
Before re-entering treated areas, operators are required to wear full-face gas masks equipped with ABEK2 Hg CO P3 or ABEK2 NO P3 filters. Since ozone’s reactivity rapidly degrades these filters, they should be inspected and replaced regularly. For environments with very high ozone levels or during emergencies, a Self-Contained Breathing Apparatus (SCBA) is recommended for complete respiratory isolation. Additionally, ozone’s oxidative properties can damage materials like rubber, neoprene, polyamide, and polypropylene. As a result, all protective gear should be carefully inspected after each use to ensure its integrity.
Conclusion
Recent studies highlight ozone’s effectiveness in achieving over 99.99% sterilization in operating rooms, making it a powerful tool for disinfection. Ozone gas excels at reaching tight, hard-to-clean areas, ensuring thorough disinfection without leaving harmful residues behind.
However, proper management is crucial. For rapid sterilization, ozone levels need to exceed 2,000 ppm within one minute, but such concentrations can present serious health risks if not carefully controlled. Disinfection must take place in a sealed environment, followed by a destruction phase – heating to 131–140°F for 20 minutes – to safely eliminate residual ozone. Pathogens vary in their resistance to ozone, with bacteria like E. coli being more easily inactivated due to their thinner cell walls.
Expert oversight is essential for safe and effective use. For example, Ozonated Cleaning LLC provides eco-friendly ozone disinfection services in the Chicagoland area, ensuring proper ozone concentration control and safe reentry into treated spaces.
Incorporating ozone disinfection into operating room cleaning routines – before the first procedure, between surgeries, and during terminal cleaning – demonstrates its practical benefits in healthcare. When paired with manual cleaning and strict safety protocols, ozone disinfection becomes a valuable method for maintaining sterile surgical environments. This makes it a key component in modern operating room hygiene practices.
FAQs
How is ozone disinfection validated in an operating room?
Ozone disinfection in operating rooms is confirmed by measuring how much microbial counts drop on surfaces and in the air. Testing before and after treatment shows a notable reduction in pathogens, bringing them down to safe levels. This process highlights its reliability and safety for sanitizing these critical environments.
How long before staff can safely re-enter after ozone treatment?
Once the ozone has completely broken down into oxygen and the space has been properly ventilated, staff can safely re-enter. Allow enough time for the area to air out thoroughly after treatment to ensure it is safe for people to occupy.
What operating room materials can ozone damage over time?
Over time, ozone exposure can cause noticeable damage to materials such as rubber, plastics, fabrics, paint, and some metals. This happens because ozone is a powerful oxidizer, breaking down and weakening these materials when they are exposed to it for extended periods.

Recent Comments